
October 25, 2019
In addition to all current open procedures, Johns Hopkins performs a high volume of transcatheter mitral valve repairs – a less invasive method using systems such as MitraClip
The past several years have seen a number of new products and procedures to treat structural heart disease conditions. Many have been for the aortic valve, such as transcatheter aortic valve replacement (TAVR), demonstrated in two pivotal trials published in 2019 to be safe in the management of aortic stenosis — even in patients with a low risk of death from surgery. Now, mitral valve therapies are having their day.
“In the mitral arena, there’s a lot going on,” says interventional cardiologist Jon Resar, medical director of Johns Hopkins’ Structural Heart Disease Program. “This is the new frontier. We’ve conquered the aortic valve, and now it’s time to move on to the mitral valve.”
Share Fast Facts
“In the mitral arena, there’s a lot going on,” says interventional cardiologist Jon Resar. “This is the new frontier. We’ve conquered the aortic valve, and now it’s time to move on to the mitral valve.” Click to Tweet

“This is the new frontier. We’ve conquered the aortic valve, and now it’s time to move on to the mitral valve.” Jon Resar, medical director of Johns Hopkins’ Structural Heart Disease Program.
In addition to open surgical approaches such as mitral valve repair or replacement that are currently available, the Structural Heart Disease Program is embracing minimally invasive, transcatheter options for mitral valve replacement and repair.
One possibility for patients with mitral valve regurgitation is transcatheter mitral valve repair (TMVR) using systems such as MitraClip. During this minimally invasive procedure, of which Johns Hopkins is a high-volume provider, cardiac specialists use a catheter, threaded up to the heart through a vein in the groin, to deliver a device that clips the two leaflets of the mitral valve together, thereby significantly reducing leaking of the valve. Echocardiographic guidance allows experts to verify the results of the procedure as they perform it.
A large clinical trial Johns Hopkins participated in, called COAPT, randomized patients with leaky mitral valves to receive optimal medical therapy alone versus optimal medical therapy with the less invasive MitraClip procedure.
“It was a revolutionary trial,” Resar says, “showing that using the minimally invasive procedure plus medical management keeps patients out of the hospital for heart failure, with a lower risk of death.” Results were published this spring in the Journal of the American College of Cardiology.
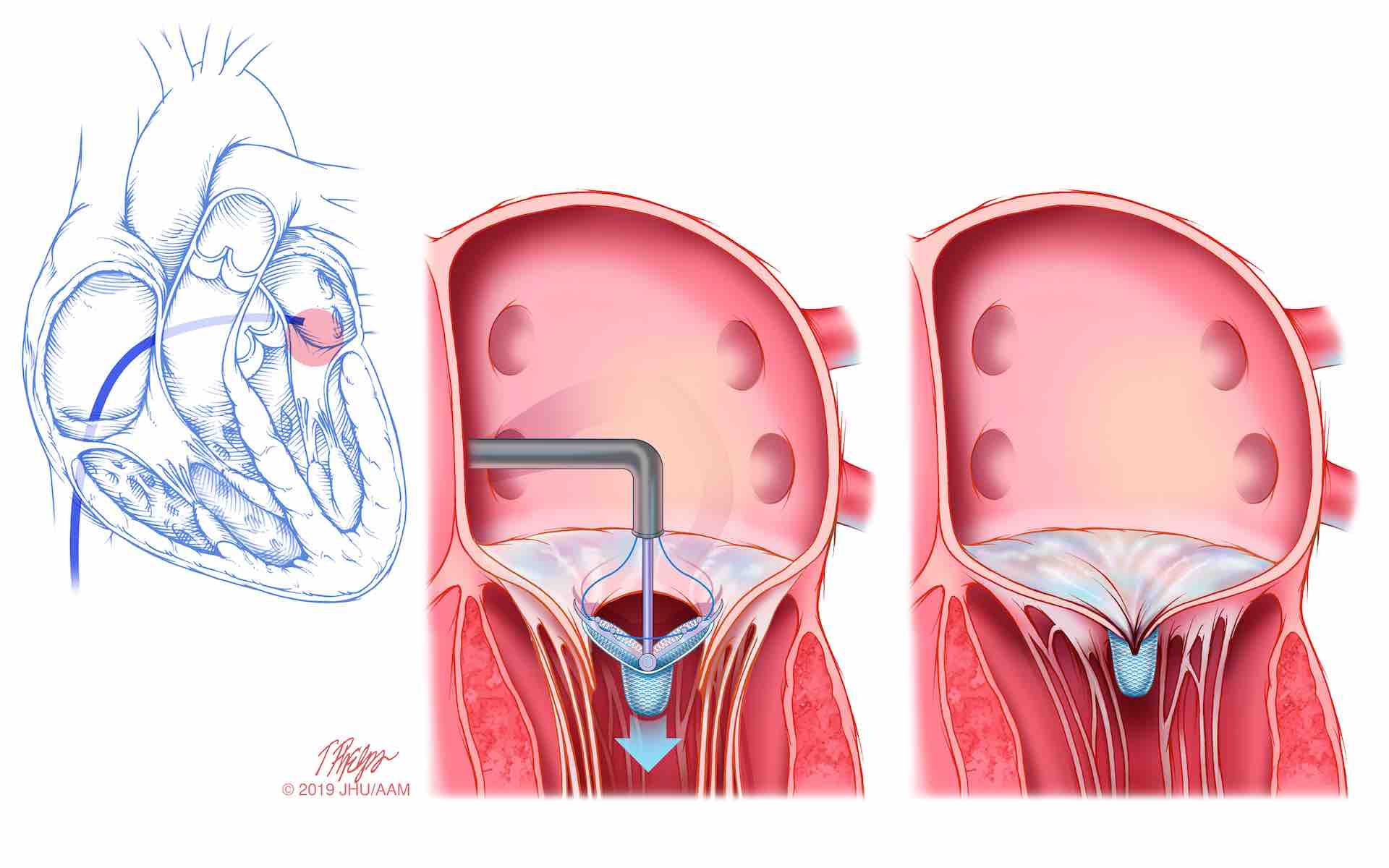
Resar and colleagues also are participating in a clinical trial of transcatheter mitral valve replacement for patients with severe symptomatic mitral regurgitation. Like TAVR, this uses a transcatheter approach to replace the leaky mitral valve with a prosthetic valve. Several patients have been treated so far at Johns Hopkins.
“The replacement valve completely eliminates mitral regurgitation,” Resar says. “We are one of about 50 hospitals worldwide participating in this study. There are a lot of other therapies in the pipeline that will be undergoing clinical trials as well.”
For referrals, please call the The Johns Hopkins Hospital Structural Heart Disease Clinic at 410-614-1132.

