Johns Hopkins Surgery
June 23, 2014
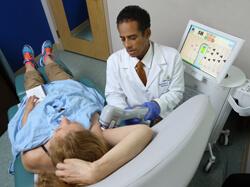
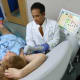
At the Johns Hopkins Center for Sweat Disorders, co-director and thoracic surgeonMalcolm Brock works with dermatologists, neurologists and behavioral medicine specialists to customize treatments for this disorder. Therapeutic options include medication, botulinum toxin injection, iontophoresis, microwave thermolysis and thoracic sympathotomy surgery.
“Conservative, temporary therapies generally begin with the least invasive, such as topical cream, and work up to more aggressive interventions such as electric currents and Botox,” says Brock.
For a permanent solution under the arms, microwave thermolysis delivers heat to the underarm sweat glands and completely eliminates them. Even though 2 percent of the body’s glands are affected, Brock says it does not hinder the patient’s overall ability to regulate temperature.
A surgical option for hyperhidrosis
Another permanent option for underarm, palm, scalp or facial sweating is thoracic sympathotomy. Over the last two decades, this procedure has evolved.
“The first sympathotomies would actually remove the sympathetic nerve,” says Brock. “Then we found that cutting the nerve would do the trick, and so we did open surgery to make the cut. Today, we do video-assisted thoracoscopic surgery.”
Since 1998, Johns Hopkins surgeons have performed hundreds of these procedures. One small incision under an arm allows a camera and a scope, as well as a valve to allow air to one lung. The other lung slowly deflates to provide a clear view of the nerve.
Depending on where the sweating occurs, newly established guidelines recommend where to sever the sympathetic nerve corresponding to the ribs: near ribs three or four for palm sweating, near ribs four or five for underarm sweating, and near rib three for facial sweating.
“Surgeons used to cut near rib two, but we now realize this can cause severe compensatory sweating, where patients may begin excessively sweating from other parts of their bodies,” says Brock. “Since going to the third rib, there are less complaints.”
While compensatory sweating can still occur, the satisfaction rates are much higher. Today, 70 to 80 percent of patients who undergo surgery for underarm and facial sweating are satisfied, and more than 90 percent of those who undergo surgery for palm sweating are happy with the results.
To refer a patient: 443-997-9328 (443-99-SWEAT)

