
April 28, 2017
Dome
Patients receive image-guided procedures sooner, with fewer trips to the radiology department.
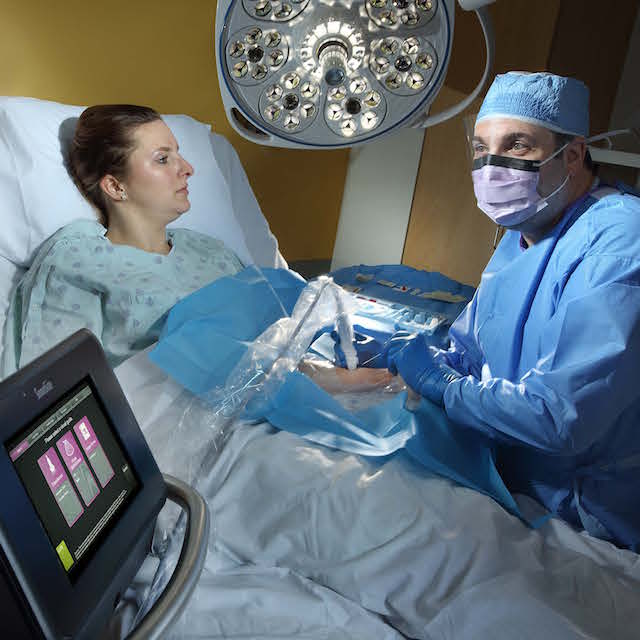
Imagine a hospitalized cancer patient who needs a central line inserted in order to receive chemotherapy. This particular patient is prone to excessive bleeding, so precision is at a premium. The oncologist requests a bedside imaging device and a physician or physician assistant who is trained to use it.
The Interventional Radiology Bedside Service, which launched Oct. 1, 2016, means patients who need these image-guided procedures have shorter waits. The new service also promotes efficient use of hospital resources because fewer patients are moved to the interventional radiology suite for procedures that can be handled at the bedside.
Some history: In 2007, The Johns Hopkins Hospital established a bedside procedure service using a point-of-care mobile imaging device so patients could stay in their rooms for image-guided procedures. In the past, these patients required transport to either a surgical suite or the interventional radiology division.
The bedside service was staffed by internist Gigi Liu and physician assistants David Lichtman and Jacob Yates, who were specially trained in the procedures and became experienced at challenges such as inserting central lines in patients who were unable to lie flat, says Lichtman. Most procedures take between 20 minutes and an hour, and include lumbar punctures, catheter insertions and using needles to remove fluid.
Meanwhile, to improve accuracy, demand for imaging to guide needles or catheters increased, outpacing the capacity of the bedside service. More patients were referred to the interventional radiology suite. That increased the burden on radiologists and created hassles for patients, who sometimes had to wait until the following day for an appointment with an interventional radiologist.
“For patients, that meant delay of care and leaving the bed to go somewhere else,” says Kelvin Hong, director of interventional radiology for The Johns Hopkins Hospital. Hong teamed with internist Carrie Herzke, associate vice chair for clinical affairs for the Department of Medicine, to propose a simpler way forward.
Their plan was to increase the capacity for image-guided procedures at the bedside by training more physician assistants in bedside procedures.
The idea won early support from Johns Hopkins Hospital President Redonda G. Miller. “This is a win-win proposition,” she says. “It provides a service to clinicians who may not have the time or training to do bedside procedures, and it’s potentially safer for our patients in certain circumstances.”
Already, two additional physician assistants have been trained to do the bedside procedures, says Hong. Capacity has increased, he says, and most procedures are now done the same day as the request.
Additional staff members and more mobile imaging devices could expand the bedside service even more, he says, to include weeknight evenings and weekends.

