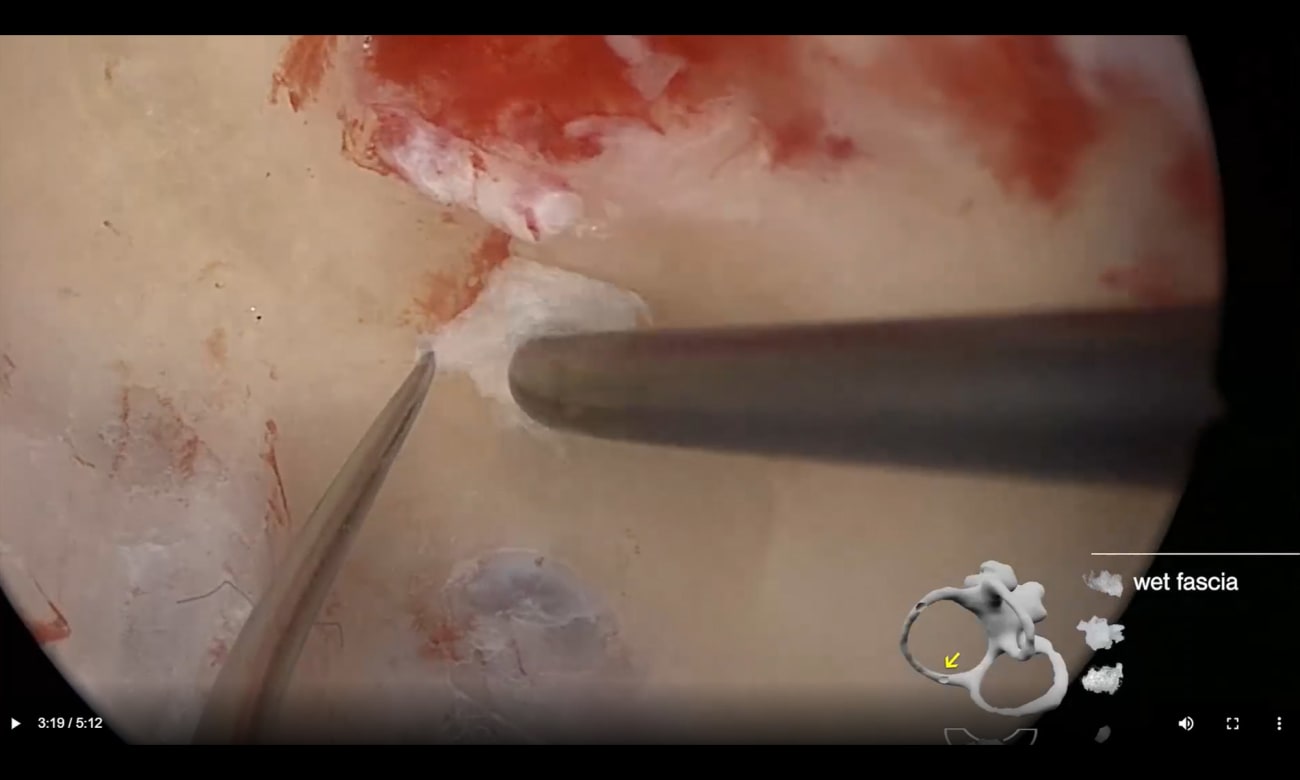
Surgeries on the inner ear always carry a risk of losing hearing and balance function, says John Carey, Johns Hopkins’ director of otology, neurotology and skull base surgery. This risk, he adds, is especially high for procedures that require opening up the semicircular canals — such as those to treat superior canal dehiscence (SCD) syndrome, a rare disease that Carey specializes in treating.
Recently, Carey and his colleagues suspected that part of the risk inherent in treating SCD was due to the loss of perilymph from opening the bony labyrinth. To solve this issue, he and his colleagues developed a new procedure that allows this surgery to occur “underwater,” using a solution with a composition as close as possible to perilymph.
To evaluate how this new procedure compares with the standard approach, Carey and his team evaluated 13 patients who underwent transmastoid repair for SCD: Six had the traditional surgery; seven had the underwater one.
“We found that our hearing outcomes with the underwater approach were better than with the standard microscopic approach,” Carey says. “So, we are happy to offer the underwater transmastoid approach, when the anatomy or other factors make this approach favorable for the patient.”

This example, Carey says, is just one of the many innovations that the Division of Otology, Neurotology and Skull Base Surgery is continually developing for patients. These research projects, including new drug vehicles for the inner ear; artificial intelligence to analyze temporal bone scans; and new MRI techniques to diagnose vestibular disorders, are improving care for patients at Johns Hopkins and beyond.
Share Fast Facts
A new @hopkins_ent procedure used to treat superior canal dehiscence allows the surgery to be performed underwater. Click to Tweet
Artificial Intelligence for Automating Data Extraction
A team led by neurotologist Francis Creighton, including otolaryngologist-head and neck surgeon Masaru Ishii, is developing new methods to automatically analyze temporal bone CT scans to determine clinically and surgically relevant anatomical measurements. Traditionally, these measurements — performed on bones so small that all would fit together on a dime — are performed by manual segmentation, a time-consuming technique that’s prone to error and significant variability between users. To solve these problems, Creighton and his colleagues are evaluating using computer vision, a type of artificial intelligence, to extract needed measurements, using machine learning algorithms. “We hope that this methodology will allow us to begin to investigate what normal and abnormal metrics are between different patient populations,” Creighton says, “and in the future allow us to automate surgical planning for robotic procedures of the ear and skull base.”
Improving Imaging for Vestibular Disorders
Otologist Bryan Ward and his colleagues are using new MRI techniques — including stronger 7T magnetic fields, new pulse sequences, and improved gradients in 3T MRI — to develop higher resolution imaging of the inner ear in patients with vestibular disorders. “My goal is to use a combination of temporal bone histopathology and better inner ear imaging to identify novel causes of inner ear vestibular disorders,” Ward says.
Recently, Ward and his team published a review of vestibular disorders that are currently diagnosed by gathering a detailed history and physical exam, but should be identifiable with better imaging techniques. These researchers also recently published a temporal bone histopathology study that identified areas of vascular vulnerability in the inner ear. Upcoming publications will focus on inner ear structures that can be seen at 3T MRI and on an explanation for discrepancies in testing results that are often seen in patients with Meniere's disease.
To refer a patient, call 443-997-6467 or email JHOtoAccess@jhmi.edu