
NeuroLogic
May 1, 2013
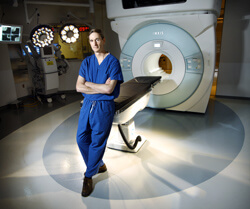
Over the years, neurosurgeons such as Jon Weingart have had an increasingly larger toolbox to distinguish normal from cancerous tissue during surgery. For example, he and other Johns Hopkins neurosurgeons use intraoperative navigation—a type of “GPS for the brain” that uses MRI images taken before surgery as its map. Because tumor tissue has a different signature on MRI, it allows surgeons to use these images as a guide to differentiate between diseased and healthy tissue during surgery.
However, Weingart says, this technology has a critical flaw: “The brain floats in water,” he points out, “so there is some shifting and changing of things between when we take preoperative MRIs and when we’re performing surgery.”
Because even minor differences can make a statistically significant difference in patients’ outcomes, he adds, it’s important to remove just the right amount of tissue. That’s the reason why Johns Hopkins included intraoperative MRI as part of the Sheikh Zayed Tower, one of The Johns Hopkins Hospital’s new clinical buildings that opened last year.
Incorporating intraoperative MRI into the neurosurgery operating room suites required some special architectural planning, Weingart says. The imaging apparatus, which is shared between two operating rooms, hangs on a track suspended from the ceiling. Both rooms are shielded, just like rooms for regular MRIs.
Using the machine also requires planning during surgery. Patients must be encased in specially designed cocoons when they enter the tunnel to keep the field sterile, Weingart explains. Also, surgical instruments are carefully counted before a scan, since metal objects are attracted to the MRI’s powerful magnet.
So far, the team has used the intraoperative MRI in more than 60 cases. In about 40 percent of those cases, surgeons ended up removing more tissue after patients received an intraoperative scan.
“That’s very significant,” Weingart says. “In nearly half of these cases, the intraoperative MRI allowed us to make a decision that could improve these patients’ outcomes.”
Weingart says that with each use of the technology, the team is gathering data to accurately measure the differences in patient outcomes compared to surgeries before intraoperative MRI was in place.
“Eventually, with enough data,” he says, “intraoperative MRI could become the standard of care.”

