

Johns Hopkins clinicians and engineers are creating a model for a safer, less costly and more productive clinical unit—that can be adopted anywhere.
Consider the infusion pump. These machines deliver vital medications and nutrients for nine out of 10 hospitalized patients. But for clinicians, they require too many steps and create too many opportunities for human error.
First, a nurse calculates dosage by typing a patient’s weight into an algorithm. The next step is checking the result with another nurse who performed the same calculation. Next, the nurse walks to the infusion machine to program it, then back to a computer to document the information in the patient’s electronic medical record.
“So much of health care is people literally carrying data from place to place,” says critical care physician Mark Romig.

- Mark Romig
That’s because the intensive care unit wasn’t designed as a system, says engineer Alan Ravitz of the Johns Hopkins University Applied Physics Laboratory (APL). “It was designed as separate little entities.”
Peter Pronovost, director of the Armstrong Institute for Patient Safety and Quality, and Ravitz, with guidance from Conrad Grant, chief engineer at APL, are leading a team at Johns Hopkins to change that piecemeal approach with a blueprint that is ambitious in scope. The researchers are laying the groundwork for the clinical unit of the future—one that will take a “systems approach” by tapping into continuous, automatically generated data from multiple sources to tailor treatments to individual hospital patients.
And their vision doesn’t stop at the walls of The Johns Hopkins Hospital.
“We are working to design an ICU that does not harm, that heals more, that costs less, that is more productive and is more joyful for staff,” says Pronovost, who is working closely with Grant, Ravitz and Johns Hopkins Medicine clinicians, including Romig, to bring this vision to reality. “And when we have it, we plan to disseminate this globally so patients anywhere in the world can get the same care as they would at the world’s top hospitals.”
Consider this: ICU patients currently require as many as 200 actions per day and 100 pieces of equipment. The information from all these actions and devices is easy for computers to digest but is far more than humans can comprehend. What’s more, much of the information is not useful because it reflects a clinician’s assessment at a single moment in time.
Project Emerge, launched in 2013 with support from the Gordon and Betty Moore Foundation, was a first step toward redesigning the workflow, culture and technology in the ICU, all in an effort to provide better information in a format that’s useful to clinicians and safer for patients.
The foundation for Project Emerge is a software tool that takes data from hundreds of sources to provide a single display on a computer tablet. Red panels indicate if actions are needed to prevent harms, such as blood clots, infection or ICU-acquired weakness. Yellow panels show upcoming actions, and green indicates those that have been completed.
Piloted in 2014 in The Johns Hopkins Hospital’s surgical ICU, the app is now being used at the University of California, San Francisco Medical Center. While the app does help clinicians comply with best practices—the time required for clinicians to ensure that a patient received every best practice went from 19 minutes to six minutes, and their assessments were 17 percent more accurate, according to Pronovost—it doesn’t yet provide the ICU-wide integration that Pronovost envisions.
In 2014, the Project Emerge team launched an effort that researches ways to integrate infusion pumps and electronic medical records. A fully integrated ICU could become reality within five years, Pronovost says, when a new ICU is built at Johns Hopkins Bayview Medical Center.
“With clinicians spending less time on documenting and gathering supplies, productivity will improve and burnout will be less common,” he says. “They will focus on what they do best—diagnosing, treating, comforting—but with the support of predictive analytics and precision medicine. The patient experience will be transformed.”
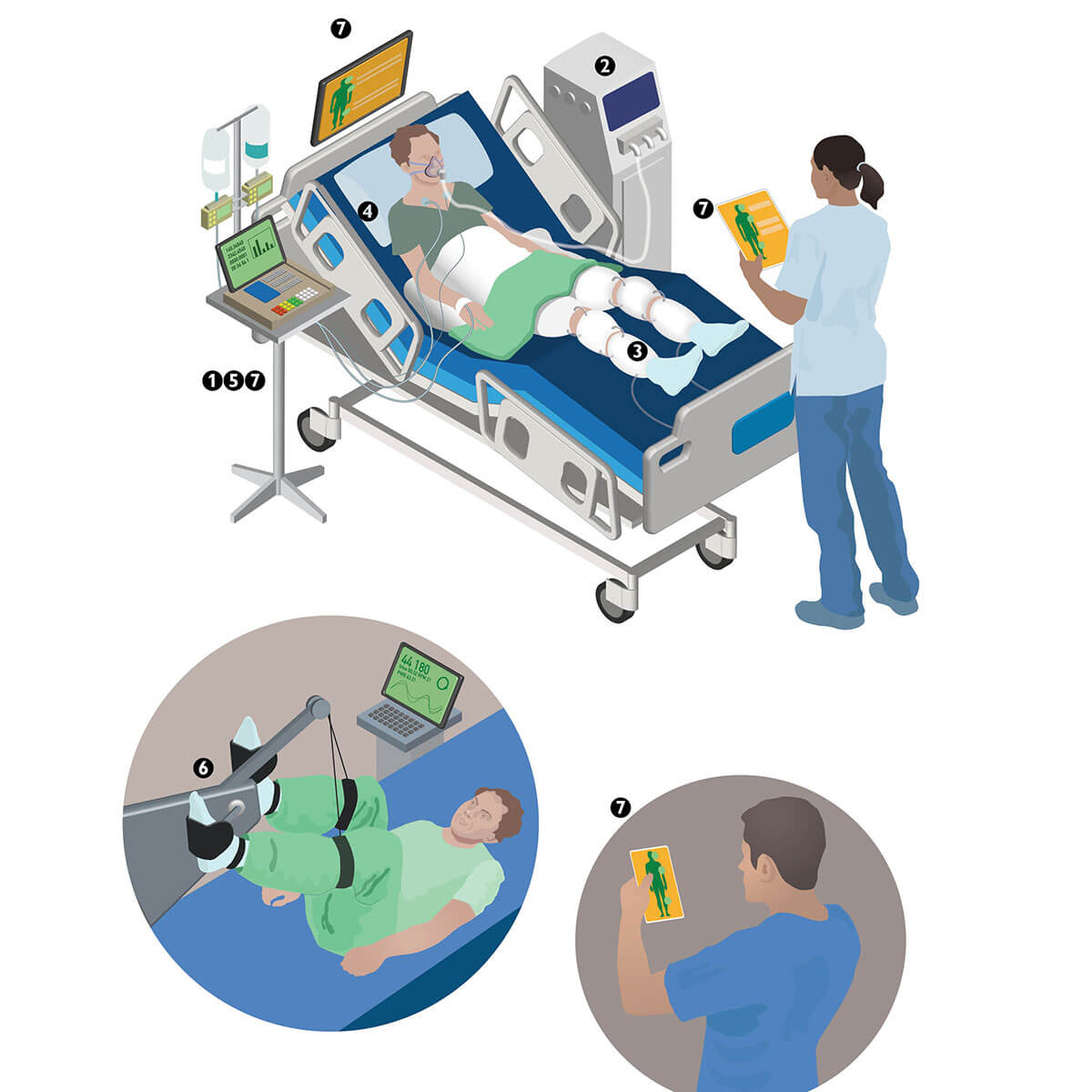
What we might see:
- Infusion pumps that eliminate manual dosage calculations and data entry
- Mechanical ventilators that continually track oxygen levels and recommend changes when necessary
- Sensors on sequential compression devices that ensure patients are wearing them and they are alternating air flow as required to prevent deep vein thrombosis
- Monitors that track optimal bed positioning so clinicians don’t have to
- A single, integrated alarm system
- Devices, such as stationary bicycles, that can fight ICU-induced weakness by monitoring when patients exercise, tracking their strength and duration, and providing that information in the patient’s record alongside vital signs, like heart rate and blood pressure
- Machine learning, which will allow these units to continually learn from one another and update their practices based on data showing what works
The vision: These modular units can be combined into integrated clinics, which can combine into integrated hospitals and hospital systems.

