InsideTract
April 26, 2017
Joanna Melia’s patients with inflammatory bowel disease all ask her the same thing.
“Every single one of them wants to know what they should and shouldn’t eat,” she says.
“Which seems reasonable, right? But there’s very little information on dietary recommendations for patients” with Crohn’s disease and ulcerative colitis.
Her research is driven by a desire to give those patients some answers.
Melia, a gastroenterologist and researcher, says some patients tell her that certain foods trigger episodes while others report diet has no affect on their symptoms.
For example, for a long time, IBD patients were encouraged to avoid foods containing fiber. “Now the pendulum is swinging the other way,” she says. “Newer studies say that fiber is good. So it’s really a moving target.”
To better understand one aspect of diet and IBD, Melia is researching a zinc transporting gene that has a mutation associated with increased risk of Crohn’s disease. The mutation has also turned up in research of several other diseases, including obesity and schizophrenia, and it might hold clues to how micronutrients in the gut affect disease.

Melia says that it may produce either too much or too little immune response in patients with IBD. Either can lead to intestinal inflammation.
“Historically, we have divided up inflammatory bowel disease into only two disease conditions, Crohn’s disease and ulcerative colitis,” says Melia. “But there are likely many subtypes driven by many different processes.”
Using enteroids grown from intestinal tissue samples, Melia and other Johns Hopkins researchers study intestinal transporters.
She says that many of her Johns Hopkins colleagues have produced important work in IBD genetics and in the area of dietary trace minerals, such as copper, iron and zinc. Melia sees herself working in that tradition.
Melia’s research also focuses on how micronutrients, required by both humans and the microorganisms present in the gut, shape the microbiome.
“There seems to be some competition among the host and organisms in the gut for these micronutrients in IBD,” she says. “For instance, we and our collaborators have found that the microorganisms in the intestines of patients with Crohn’s disease have more zinc transporters than the ones in healthy people.”
The role of diet in shaping the microbiome is undeniable, Melia says. But exactly what effects various foods produce remains elusive. Still, she believes there is hope to unlocking the puzzles of IBD, diet and the microbiome.
“We really want to learn how we can harness micronutrients to improve gut health. I think we have new laboratory tools to begin to study these questions in new ways, and it is my hope we can provide more answers for patients,” she says.
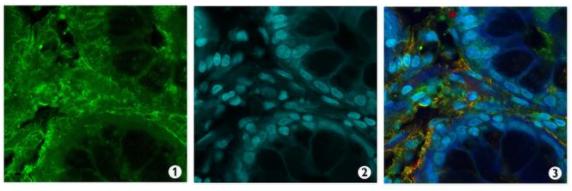
In this colocalization of a specimen taken from a patient with ileal Crohn’s disease, a green stain in image 1 illuminates zinc transporter genes within the instestinal crypt cells. Image 2 shows the cells’ teal-stained nuclei. Image 3 overlays the other two images and highlights in red a special type of crypt cell. “This tells us that the zinc transporter is present in some of the immune cells in the epithelia of both the terminal illium and the small bowel,” says researcher Joanna Melia, “and that there is even more of it in the presence of inflammation.”